Orthodontics and Cone-beam Computed Tomography: Improved Diagnosis and Treatment Outcomes
A significant aspect of treating patients in orthodontics is providing education about the need for treatment and the processes necessary for successful outcomes. Bridging that gap between patient understanding and dental and orthodontic best practices is the goal. New diagnostic tools such as 3D or cone-beam computed tomography (CBCT) are improving diagnosis and treatment outcomes.
CBCT provides greatly enhanced, three-dimensional images of designated regions of the head, jaw and sinuses. Some dental practitioners and especially orthodontists now use 3D imaging exclusively in their practices because CBCT affords better overall diagnostic information, especially on positioning and relative health of the teeth, gums and airways, than more traditional 2D imaging.
The Journal of the American Dental Association website describes the technical process of CBCT this way: “A CBCT scanner uses a collimated x-ray source that produces a cone or pyramid-shaped beam of x-radiation, which makes a single full or partial circulation revolution around the patient, producing a sequence of discrete planar project images using a digital detector. These two-dimensional images are reconstructed into a three-dimensional volume that can be viewed in a variety of ways, including cross-sectional images and volume renderings of the oral anatomy.”
The specificity of CBCT is important as well in interpreting relationships between hard and soft tissues. Information at that level improves the ability to deliver the right diagnosis leading to better treatment and a more effective orthodontic practitioner.
Just as significantly, CBCT is both fast and convenient, providing images within minutes that can be used to explain and explore options to patients and even emailed or shared with family members via the Internet. The continued advances in 3D imaging and digital technology make it practical to generate and employ high-grade diagnostic information from the start of treatment through documentation of outcomes.
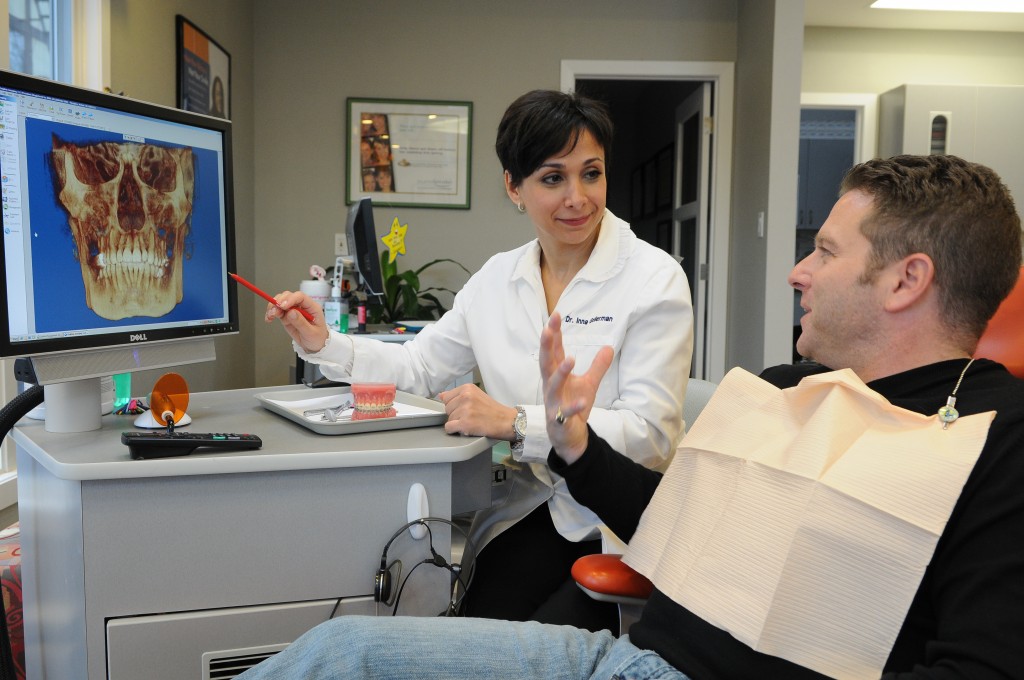
The level of enhanced understanding and communication with patients cannot be overstated. Being able to share the three-dimensional view, including position of teeth in the skull and jaw, as well as impacts from misplaced or misaligned teeth is easier to explain when the evidence is presented like an image on TV.
Orthodontic problems such as tooth impactions can be shown in full spectrum. Asymmetries, midlines and other aspects can be measured even without the patient present. Images can also be manipulated to various angles to provide diagnostic perspective. Orthodontists can look at the face from any angle thanks to the three-dimensional information provided by CBCT.
CBCT devices were first introduced commercially in the United States in 2001. Since then their use has grown in the greater dental community. So what are the potential drawbacks? Primarily there is professional concern about the dose of radiation delivered during the actual CT scan, which the FDA touches on in its Initiative to Reduce Unnecessary Radiation Exposure from Medical Imaging.
Dental CBCT is considered a highly valid diagnostic protocol that provides superior information than methods such as two-dimensional x-rays that have been the standard for years. Radiation doses from CBCT exams are generally lower than broader-based CT exams, but do require more radiation exposure than 2D dental x-rays. That means dental practitioners must address the frequency of use in the overall treatment pattern for the patient. The long-term perspective is also important to consider, as younger patients still face a lifetime of clinical treatment protocols that may put them at risk for increased radiation exposure.
The ADA Council on Scientific Affairs states that it promotes “safe use of cone-beam computed tomography (CBCT) and appropriate professional justification of CBCT imaging procedures.” Use of CBCT scans should always be considered in context with their value at a particular point in a patient’s life and development. The ADA recommends reviewing a patient’s health and imaging history and assessing that the potential clinical benefits outweigh risks associated with exposure to ionizing radiation. Of course, adequate and appropriate training is a must for all dental professionals employing CBCT in their practices.
In balance with these recommendations and rules, CBCT opens new potential for clear and compelling diagnostic conclusions. Some CBCT units even offer the capability to produce movies illustrating the mouth in context with the head and skull.
CBCT can also enable dentists, orthodontists and other practitioners the ability to reduce patient discomfort using nerve-marking interactive tools to locate and isolate the nerve canal on a panoramic projection. The same level of inspection is assistive in analyzing the temporomandibular joint for TMJ problems. Analysis can include coronal, sagittal and circular analysis of the area.
CT scans have long been considered a lifesaver for diagnosis of cancers and other illnesses. The use of CBCT in dental and orthodontic practices holds potential to revolutionize the understanding and treatment of patient dentition to create better outcomes. That is a picture everyone can appreciate and enjoy.

The long-term perspective is also important to consider, as younger patients still face a lifetime of clinical treatment protocols that may put them at risk for increased radiation exposure.
It seems cool to see a lot of new dental technology especially the CBCT scanner. I hope that these technology are available in other countries so that more people can benefit from it. If these technologies were invented earlier then I would not have misaligned teeth, which was caused by my childhood dentist.
Use of cone-beam computed tomography in dental practice is gaining its popularity day by day. It makes diagnosis process more easy. It helps oral healthcare professional to diagnose oral disease properly which in turn helps patient to get better treatment.
What I admire the most about the team at Precision Esthetics is that they truly enjoy what they do. Their products are made at the highest quality possible. My patients expressed satisfaction in the implant cases that were fabricated for them. I’m a Prosthodontist in New York and all my orders are delivered to my office on time. You should check out their website http://www.precisionesthetics.com or call (800) 942-3368. I highly recommend them to any dental professional looking for the best in the business.
Thanks for sharing this info
I really like that you are using state of art tectnology like CBCT in orthodontic practices. Yes thisreally has the potential to revolutionize the treatment of patient dentition to create better outcomes.